Handling Patient Complaints Legally & Professionally
Patient complaints test the real strength of a medical office. They expose whether the team can protect trust under pressure, preserve privacy while emotions rise, document facts cleanly, and move a tense interaction toward resolution without creating extra risk. A rushed answer, a defensive tone, or a careless note can turn a routine complaint into a compliance problem, a billing dispute, a privacy concern, or a long-term reputation hit.
This guide breaks the process into the steps that matter most: complaint triage, staff language, documentation discipline, privacy protection, escalation triggers, and follow-up systems. Offices that train around active listening techniques, strengthen de-escalation techniques, tighten patient privacy communication essentials, and improve effective patient communication terms handle complaints with far less chaos and far more control.
1. Understand Which Complaints Carry Legal Risk And Which Ones Demand Immediate Escalation
Every complaint deserves respect. Some complaints also demand fast escalation because the office is dealing with more than frustration. Privacy concerns, record-access disputes, discrimination allegations, threats, safety events, consent confusion, billing irregularities, and staff-behavior complaints can all create exposure if the response is casual or poorly documented. Teams that know the language of top 20 HIPAA and patient privacy terms, understand patient intake procedures, follow strong front-desk operations terms, and use better healthcare portal terms recognize risk sooner and respond with more precision.
A useful first move is categorization. Ask whether the complaint is primarily about communication, access, scheduling, privacy, records, clinical documentation, billing, staff conduct, or safety. That single decision shapes who should own the case, what must be documented, which system should hold the record, and how fast the office must act. Training becomes far stronger when staff review top 20 scheduling and appointment terms, learn insurance verification definitions, sharpen healthcare CRM terms, and practice interactive guide to handling appointment scheduling conflicts, because a complaint often starts in one lane and spills into three others.
Legal risk also rises when staff speak before they understand the facts. Patients often open with conclusions: “You violated my privacy,” “You billed me illegally,” “Your staff refused care,” “My record is wrong,” “You lost my paperwork.” The professional response is careful acknowledgment, fact gathering, privacy control, and internal escalation when the issue crosses a threshold. Offices that reinforce step-by-step guides for managing difficult conversations with patients, strengthen empathy in healthcare administration, improve best collaboration tools for medical office teams, and use safer patient communication apps stay calmer because the team has a process ready before the complaint arrives.
The highest-risk complaints share one trait: they can worsen through delay. A privacy complaint needs preserved facts. A chart-correction complaint needs document review. A discrimination complaint needs management attention. A threat needs safety procedures. A billing complaint tied to authorizations or coverage may need payer review before the patient receives an inaccurate answer. Staff who train with interactive training on patient record updates and EMR compliance, use tools for efficient medical records release, understand resolving common EMR software issues, and work from clear secure patient scheduling tools reduce confusion because ownership is clearer from the first minute.
2. Use A Front-End Response Sequence That Protects Privacy, Preserves Facts, And Lowers Emotion
The first thirty seconds matter more than most offices realize. A patient complaint arrives with emotion, incomplete facts, and a strong need to be taken seriously. The staff member receiving it needs a stable sequence: acknowledge, move to privacy, listen fully, clarify the actual issue, identify urgency, document objectively, and route correctly. Offices that train with appointment scheduling best practices, reinforce emergency appointment management, strengthen patient communication apps, and sharpen active listening techniques respond with structure instead of improvisation.
A professional opening sounds calm and specific. “I hear your concern.” “I want to understand exactly what happened.” “Let’s step to a private area so we can talk appropriately.” “I’m going to document the concern and make sure the right person reviews it.” That language keeps the conversation moving without admitting facts that still need investigation. Staff become much more consistent when they practice effective patient communication terms, review patient privacy communication essentials, apply de-escalation techniques, and use step-by-step guidance for difficult patient conversations.
Privacy control should happen early. A complaint about billing, behavior, records, or portal access can spill personal information into a public lobby within seconds. Bring the conversation to a quieter location, lower your own voice, confirm identity before discussing account details, and limit the audience to people who genuinely need to participate. That discipline grows when teams understand healthcare portal terms, know tools for efficient medical records release, train on EMR integration tools every medical administrative assistant needs, and use reliable secure patient scheduling tools.
Clarification is where good handlers separate themselves. Ask what happened, when it happened, who was involved, what the patient expected, and what outcome they want now. Ask short questions. Let the patient finish. Repeat the issue back in neutral language so the patient can confirm or correct it. Strong teams build this skill through healthcare CRM terms and workflows, cleaner front-desk operations, better medical admin time-tracking tools, and smarter best collaboration tools for medical office teams, because complaint handling improves when information moves cleanly across roles.
The final move in the first-contact sequence is ownership. Patients lose trust when they tell the full story and leave without a clear next step, a responsible party, or a timeline. Give a realistic follow-up window, identify who will review the concern, and record the handoff in the right system. Offices become stronger here when staff train on medical office automation trends, use directory of medical admin staff scheduling tools, practice interactive guide to emerging medical admin technologies, and learn from new study on how certified medical administrative assistants improve healthcare efficiency. Complaints cool down when the patient can see that the office has entered a controlled process.
3. Document Complaints Objectively So The Record Helps You Later Instead Of Hurting You
Complaint documentation needs discipline. The goal is a clean factual record of what was reported, what the office observed, what immediate action was taken, where the issue was routed, and what follow-up is due. Emotion-heavy wording, speculation, sarcasm, blame, and personal conclusions can damage the usefulness of the record fast. Offices that drill on interactive training for patient record updates and EMR compliance, reinforce top 20 EMR and charting terms, improve resolving common EMR software issues, and use top 10 EMR shortcuts to boost CMAA productivity document faster and cleaner when the pressure is real.
A useful complaint note usually includes six elements: date and time, source of complaint, exact concern in neutral language, people involved, immediate response, and next action. Add direct quotes only when the exact wording matters, especially for threats, allegations, or statements about privacy or discrimination. Use observable facts for behavior descriptions. “Patient spoke loudly and interrupted staff three times” is useful. “Patient was impossible” weakens the record. Teams improve when they study top 20 terms medical scribes must master for accurate clinical documentation, sharpen medical terminology mastery, strengthen annual report on documentation accuracy, and use top 100 specialty-specific documentation template libraries as models for precision.
Staff also need to know where complaint information belongs. Care-relevant facts may belong in the chart when they affect treatment, access, safety, or continuity. Service recovery notes, staff coaching details, and internal review steps may belong in the designated complaint or incident workflow according to office policy. That separation protects clarity. Teams handle this better when they understand tools for efficient medical records release, use healthcare CRM terms, manage secure communication through patient communication apps, and apply patient privacy communication essentials during follow-up.
Preservation matters too. Save portal messages, voicemails, screenshots, scheduling records, coverage-verification notes, records-release requests, and any relevant staff messages according to policy. A complaint becomes easier to resolve when the office can reconstruct the timeline quickly. That is why strong teams pair insurance verification fluency, appointment-scheduling best practices, directory tools for staff scheduling, and best collaboration tools for medical office teams with a defined complaint archive process. Fast access to facts changes the quality of every response.
4. Handle The Most Common Complaint Scenarios With Scripts That Stay Calm, Clear, And Safe
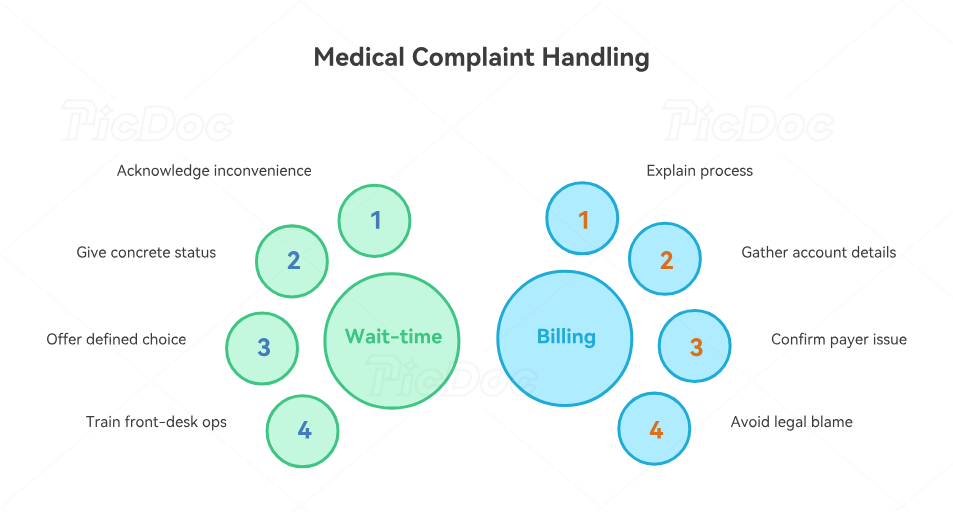
Wait-time complaints are common, and they often become disrespect complaints when staff disappear or offer vague updates. The most effective script acknowledges the inconvenience, gives a concrete status point, and offers the patient a defined choice when possible. “I understand the delay has been frustrating. I checked your status, and the current estimate is about twenty minutes. I can update you again in ten minutes, or I can ask the team whether rescheduling is a better option.” Offices improve these conversations when they train on front-desk operations, strengthen appointment scheduling best practices, use interactive guide to handling appointment scheduling conflicts, and keep staff steady with active listening techniques.
Billing complaints require especially careful language. Staff should explain the process, gather account details, confirm the payer or statement issue, and route the review without announcing legal conclusions or blame. “I can see why this balance concerns you. I’m going to verify the insurance information and ask our billing team to review the charge path before I tell you what happened.” That wording protects credibility. Teams handle these cases better when they know top 20 medical billing terms, understand insurance verification, use patient communication apps, and follow clean healthcare CRM workflows.
Chart-error complaints should be handled with precision and respect. Patients often feel deeply unsettled when their record contains the wrong medication, diagnosis, allergy, demographic detail, or visit history. The correct move is to identify the disputed field, capture the patient’s wording, follow the designated correction process, and escalate urgency if the issue affects upcoming care. Offices become safer here when they work from interactive training on patient record updates and EMR compliance, use EMR integration tools, troubleshoot with practical EMR issue guides, and reinforce charting-term clarity.
Privacy complaints deserve a slower pace and tighter control. Move the discussion away from others, verify identity, avoid overexplaining before facts are gathered, and route to the appropriate privacy or management review path. A stable response sounds like this: “I understand you are concerned about how your information was handled. I’m going to document exactly what you observed and make sure the right reviewer examines it promptly.” Offices perform much better in these moments when staff train on top 20 HIPAA terms for medical administrative assistants, review top 20 must-know HIPAA terms for medical scribes, strengthen patient privacy communication essentials, and use reliable tools for records release.
Complaints about staff conduct require both service recovery and internal accountability. Staff at the front line should gather the details without defending a coworker, attacking a coworker, or arguing about intent. “I’m sorry this interaction left you feeling disrespected. I want to understand what was said and who was involved so the concern reaches the correct supervisor.” That approach protects the office and the patient relationship at once. Teams strengthen this skill when they practice de-escalation techniques, use step-by-step difficult conversation guides, build empathy through empathy in healthcare administration scenarios, and coordinate through best collaboration tools for medical office teams.
5. Turn Complaints Into Process Improvement Without Turning Every Case Into A Crisis
Strong offices do more than close complaints. They study them. Repeated complaints about phone tone, scheduling confusion, portal delays, records release, insurance surprises, or privacy at the front desk point to process weakness. Complaint logs should reveal patterns by category, location, staff role, payer, and time of day. Teams who review medical office automation trends, adopt smarter emerging medical admin technologies, sharpen top 10 skills employers look for in a CMAA, and use medical admin time-tracking tools can spot preventable friction much faster.
The best weekly review asks practical questions. Which complaint type rose. Which step failed first. Which issues should have been resolved at the first contact. Which complaints included privacy risk. Which complaints involved poor documentation. Which staff groups need new scripts or system support. That review grows stronger when leadership leans on medical administration conferences and workshops, connects teams with medical admin professional organizations, encourages problem-sharing through online communities and forums for CMAAs, and builds repeatable improvement through future-proofing your CMAA career essential skills for 2030.
Complaint metrics become useful when they are specific. Track complaint-to-first-response time, complaint-to-resolution time, repeat complaint rate, privacy-related complaint rate, unresolved chart-correction backlog, scheduling-conflict recurrence, patient-statement confusion rate, and percent of complaints requiring leadership escalation. Offices that align these measures with interactive salary calculator for medical administrative assistants, medical admin assistant job market outlook, real-life success stories from certified medical administrative assistants, and why CMAA certification boosts career opportunities reinforce the message that complaint handling is a career-level skill, not side work.
Training should stay close to real cases. Take one complaint from the week, strip identifiers, and walk the team through the exact sequence: first contact, privacy control, note quality, escalation decision, follow-up message, and closure. Then identify the earliest preventable miss. Offices that support this learning through ultimate guide to passing your CMAA certification exam, interactive CMAA practice exam, essential study tips for exam success, and complete breakdown of what is included in the 2026-27 CMAA exam build better judgment because the training mirrors the actual work.
6. Frequently Asked Questions About Handling Patient Complaints Legally & Professionally
-
The first move is controlled acknowledgment and privacy protection. Recognize the concern, lower the temperature, and move the conversation away from public traffic if possible. Then gather facts in a calm sequence instead of rushing into explanations. Offices handle this far better when staff train on de-escalation techniques, strengthen active listening techniques, improve front-desk operations, and apply patient privacy communication essentials.
-
Document date, time, source, core issue, involved parties, immediate response, and next step in neutral language. Use direct quotes only when precise wording matters. Focus on observable facts and avoid emotional labels or personal judgments. Teams get stronger here through interactive training on patient record updates and EMR compliance, top 20 EMR and charting terms, resolving common EMR software issues, and documentation-accuracy training.
-
Privacy concerns, threats, discrimination allegations, serious record-integrity issues, unsafe-environment complaints, and complaints that touch urgent care access deserve rapid escalation. So do disputes involving authorizations, records release, or possible misrouting of patient information. Offices classify these cases more accurately when staff understand HIPAA and privacy terms, use records-release tools, follow healthcare portal workflows, and practice step-by-step difficult conversation management.
-
Avoid announcing conclusions before the facts are reviewed. Avoid blame, sarcasm, defensive language, and casual guesses about what another department did. A stable response acknowledges the concern, promises review through the proper process, and explains the next step clearly. This skill improves through effective patient communication terms, insurance verification training, top 20 medical billing terms, and patient communication apps.
-
The biggest gains come from pattern review. Track complaint types, escalation rates, staff roles involved, and the first workflow point where the issue became preventable. Then retrain with real scenarios and update scripts, routing rules, or system settings. Offices get more leverage from this work when they use medical office automation trends, best collaboration tools for medical office teams, medical admin time-tracking tools, and interactive guide to emerging medical admin technologies.
-
Because complaint handling sits at the intersection of communication, privacy, workflow judgment, documentation, and operational leadership. A staff member who can calm tension, preserve facts, protect patient trust, and route issues correctly becomes valuable fast. That is why this skill aligns so well with CMAA career roadmap from entry-level to medical office manager, why CMAA certification dramatically boosts career opportunities, top 10 skills employers look for in a CMAA, and future-proof your CMAA career emerging skills for the next decade.