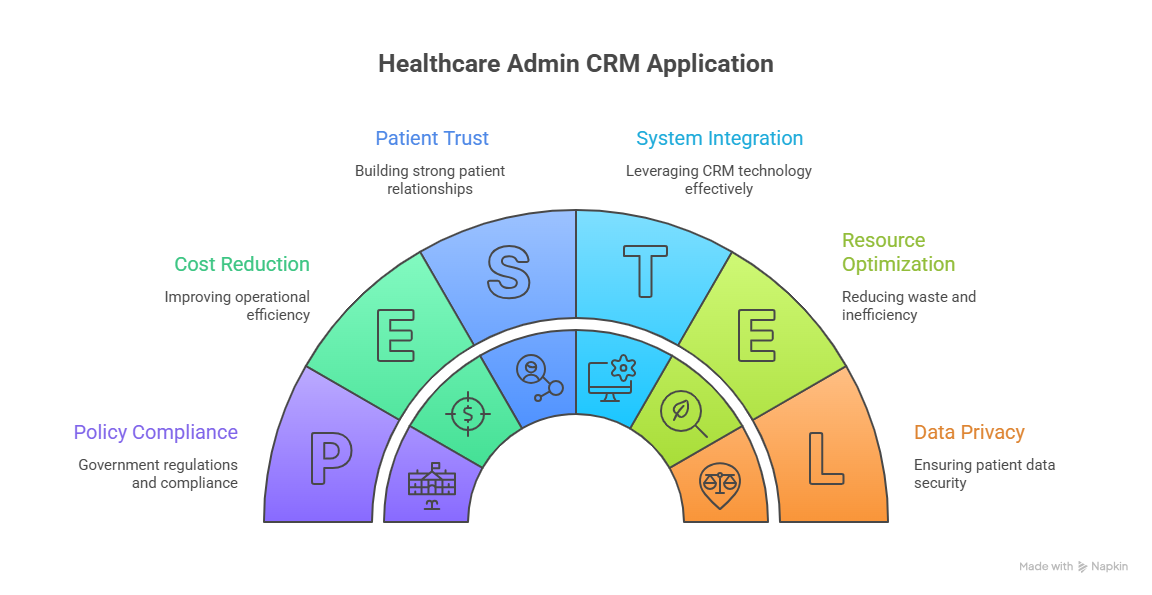
Healthcare CRM Terms: Comprehensive Interactive Reference
Healthcare CRMs are no longer “nice-to-have” software—they’re the backbone for patient relationship continuity, no-show reduction, referral capture, recall campaigns, intake completion, and service recovery after complaints. When CRM terms are misunderstood, teams misconfigure workflows, lose patients in handoff gaps, and create the exact chaos patients hate: repeated questions, missed callbacks, unclear next steps, and “we never got that form.” This comprehensive interactive reference turns CRM language into practical, day-to-day operating clarity—especially for ACMSO learners building modern, tech-enabled healthcare administration skills.
1: What a Healthcare CRM Really Does (and Why Misunderstanding Terms Causes Patient Leakage)
A healthcare CRM is not just “a database” or “a texting tool.” It is the system (or system layer) that manages patient interactions across channels—phone, portal, email, SMS, referrals, campaigns, call center workflows, and follow-up tasks—so patients do not fall through cracks. If you’re training for high-value admin roles, CRM fluency is quickly becoming as essential as knowing your EMR basics, which is why it pairs naturally with EMR software terms interactive dictionary & walkthroughs, patient management systems interactive dictionary & examples, scheduling software glossary interactive guide & tutorials, and medical office automation trends opportunities for CMAAs.
The pain point most clinics feel is not “we don’t have patients.” It’s patient leakage: missed calls, unanswered voicemails, abandoned intake, referrals that never convert, prior-auth steps that stall, and follow-ups that slip. Those problems are usually rooted in unclear CRM ownership and confusing terminology—people use “lead,” “patient,” “contact,” “account,” “case,” and “ticket” interchangeably and then wonder why the workflow breaks. That same operational discipline is what separates high-performing admin teams in new study how certified medical administrative assistants improve healthcare efficiency, medical administration workforce trends key findings for 2025, virtual medical administration how remote work is transforming the role, and interactive guide the medical office of 2025 technologies CMAAs must master.
A CRM becomes powerful when it does four things consistently:
Captures demand (inquiries, referrals, web forms, call center interactions).
Routes work (tasks, assignments, queues, escalations).
Tracks outcomes (conversion, attendance, revenue, patient satisfaction).
Automates follow-up (recalls, reminders, reactivation, care gaps, service recovery).
These functions directly influence the patient experience skills covered in active listening in healthcare terms & interactive scenarios, medical office telephone etiquette interactive dictionary & examples, patient flow management terms interactive guide & scenarios, and patient advocacy essential terms & interactive role-play scenarios.
This guide is built like an “interactive dictionary” because CRM success is not about memorizing definitions—it’s about knowing how each term maps to a real admin action, real compliance constraints, and real patient expectations. That’s also why CRM fluency becomes a career lever for ACMSO learners aiming at growth pathways such as CMAA career roadmap from entry-level to medical office manager, top 10 skills employers look for in a CMAA, medical admin assistant job market outlook key trends for 2026-27, and why CMAA certification dramatically boosts your career opportunities.
2: CRM Language That Directly Impacts Front Desk, Scheduling, and Patient Follow-Up
If you’re a CMAA or admin professional, the CRM terms that matter most are the ones that shape everyday patient flow: scheduling adherence, phone handling, and follow-up completion. These terms also intersect heavily with “human” skills—tone, empathy, clarity—covered in medical office telephone etiquette interactive dictionary & examples, active listening in healthcare terms & interactive scenarios, conflict resolution in medical admin interactive dictionary, and patient advocacy essential terms & interactive role-play scenarios.
Contact vs patient vs guarantor (why this confusion breaks everything)
In many CRMs, a “contact” is a person record—but not every contact is the patient. Pediatrics, elderly care, and disability support create common scenarios where the caller is a caregiver but the patient is someone else. If you don’t separate those roles, you will:
Text the wrong person
Confirm appointments with the wrong contact
Record inaccurate preferences
Trigger privacy risks
This privacy and identity precision is tightly linked to the compliance mindset behind predicting HIPAA updates & how they will impact CMAAs, CMAAs & data privacy future regulations explained clearly, future healthcare compliance changes how CMAAs can prepare now, and facility safety & emergency procedures interactive dictionary.
Pipelines, stages, and dispositions (your visibility into “where patients disappear”)
When clinics complain “patients don’t respond,” it often means the clinic cannot see what stage the patient is stuck in. A pipeline makes the journey visible: inquiry → verify → schedule → confirm → complete. Dispositions then capture outcomes after each attempt (“left voicemail,” “scheduled,” “needs documents,” “wrong number”). This aligns with operational improvement thinking found in patient flow management terms interactive guide & scenarios, patient management systems interactive dictionary & examples, scheduling software glossary interactive guide & tutorials, and medical office automation trends opportunities for CMAAs.
Tasks, queues, and SLAs (how you stop “I thought someone else handled it”)
This is the most common admin failure pattern: shared responsibility with no explicit ownership. A task must have:
Owner
Due time
Clear next action
Escalation rule when overdue
When tasks live in a monitored queue and are governed by SLAs (response-time standards), patient trust rises because they get predictable follow-through. These habits are core to high-performing admin teams described in new study how certified medical administrative assistants improve healthcare efficiency, medical administration workforce trends key findings for 2025, virtual medical administration how remote work is transforming the role, and how CMAAs will lead the patient experience revolution by 2030.
Consent management (why “we text patients” can become a compliance problem)
Healthcare communication must respect consent boundaries and channel preferences. Consent management is where you track:
SMS opt-in/opt-out
Preferred contact method
Authorized contacts
Communication restrictions
This is not optional professionalism—it’s risk control that supports future-focused compliance readiness from future healthcare compliance changes how CMAAs can prepare now, predicting HIPAA updates & how they will impact CMAAs, CMAAs & data privacy future regulations explained clearly, and telehealth regulation changes essential insights for CMAAs.
CRM language is not “tech talk.” It is the vocabulary of reliable patient follow-up and modern administrative credibility.
3: Workflow-Critical CRM Concepts: Automation, Segmentation, and Closed-Loop Follow-Up
Most clinics buy software hoping it will “fix operations.” It doesn’t—unless the team understands how to build and run workflows inside it. The terms below are the ones that drive results (and the ones that cause embarrassment when teams misuse them).
Segmentation (targeting without spamming)
Segmentation is how you group patients for relevant outreach. Done right, it reduces patient annoyance and increases response:
“Overdue annual wellness visits”
“New patients with incomplete intake”
“Patients who no-showed twice”
“Patients with language preference Spanish”
“Referrals received but not scheduled”
Segmentation is also a patient experience skill because relevance feels respectful. It ties closely to the patient-centered communication mindset in patient advocacy essential terms & interactive role-play scenarios, active listening in healthcare terms & interactive scenarios, medical office telephone etiquette interactive dictionary & examples, and conflict resolution in medical admin interactive dictionary.
Triggers and automation rules (where results come from)
A trigger is an event that starts an action:
Referral received → create verification task
Appointment scheduled → send intake link
Intake incomplete → send reminder
Missed appointment → create reschedule task + message
Lab order placed → follow-up reminder window
Automation rules then execute tasks and messaging consistently. This is exactly where modern admin roles are evolving, which is why it aligns with why automation is the biggest opportunity for CMAA career growth, medical office automation trends opportunities for CMAAs, 10 emerging technologies every CMAA must prepare for in 2025, and how AI will transform medical administrative assistant roles by 2030.
Drip sequences (how you prevent intake and referral drop-offs)
A drip sequence is a timed message series. The point is not marketing—it’s completion. Example:
Day 0: send intake link + “what to bring”
Day 2: reminder + offer help
Day 5: final reminder + phone option
This is particularly effective in high-friction environments like new patient onboarding, imaging prep instructions, and telehealth setup—areas often discussed in telehealth expansion how it’s changing medical admin roles right now, virtual medical administration how remote work is transforming the role, predictive insights how certified CMAAs are transforming telemedicine & virtual healthcare, and the future of EMR systems what CMAAs need to know now.
Closed-loop referral (how you become a “referrer-friendly” organization)
Closed-loop referral means you track referral receipt, scheduling, visit completion, and communicate status back to referrers. Without it, referrals stall and referrers stop trusting your operation. It’s a growth engine disguised as a workflow term. This is also why CRM fluency supports advancement paths in CMAA career roadmap from entry-level to medical office manager, future-proof your CMAA career emerging skills for the next decade, interactive career planner future healthcare roles for CMAAs, and medical admin assistant job market outlook key trends for 2026-27.
These terms are not abstract—they determine whether patients experience your clinic as organized or exhausting.
4: How Healthcare Admin Teams Should Apply CRM Terms in Real Situations (Scripts, Checklists, and Handoffs)
Knowing definitions is step one. Step two is applying them in the moments that decide patient trust: phone calls, scheduling, referral coordination, billing confusion, and service recovery. This is where CRM language becomes “behavior.”
Use a simple “CRM handoff checklist” after every meaningful interaction
A high-value admin habit is to end each interaction by asking:
What is the next action? (task)
Who owns it? (assignment)
When is it due? (SLA / due date)
What is the outcome label? (disposition)
What channel is allowed? (consent / preference)
This aligns with quality communication practices taught through medical office telephone etiquette interactive dictionary & examples, active listening in healthcare terms & interactive scenarios, patient flow management terms interactive guide & scenarios, and patient management systems interactive dictionary & examples.
Front desk: turning chaos into clarity with dispositions and next steps
If a walk-in can’t be seen, the CRM should reflect the outcome clearly:
Disposition: “No same-day availability”
Task: “Call patient with next opening”
Stage: “Needs scheduling”
Consent: confirm preferred channel for follow-up
This avoids future confusion and prevents repeat complaints—a key operational benefit emphasized in how CMAAs will lead the patient experience revolution by 2030, medical office automation trends opportunities for CMAAs, new study how certified medical administrative assistants improve healthcare efficiency, and medical administration workforce trends key findings for 2025.
Scheduling: pipelines that reduce no-shows
No-shows are often not “patient irresponsibility.” They’re broken confirmation systems:
Appointment scheduled but intake incomplete
Prep instructions never received or understood
Wrong phone number
No reminder timing strategy
CRM terms like drip sequences, triggers, and segmentation become the no-show reduction toolkit when combined with strong scheduling knowledge from scheduling software glossary interactive guide & tutorials, patient flow management terms interactive guide & scenarios, the future of EMR systems what CMAAs need to know now, and telehealth expansion how it’s changing medical admin roles right now.
Referrals: closed-loop systems that win long-term growth
Referral coordinators should use a referral pipeline:
Referral received → verify coverage → schedule → visit completed → notify referrer.
When teams skip tracking, they lose referrals without noticing. This is why CRM fluency is a strategic growth skill for aspiring leaders in CMAA career roadmap from entry-level to medical office manager, future-proof your CMAA career emerging skills for the next decade, interactive career planner future healthcare roles for CMAAs, and annual CMAA job market report where demand is highest.
Service recovery: cases and audit trails that protect trust
When a patient complaint occurs, teams often scramble because there’s no clean record of what happened. A case-based workflow with an audit trail prevents “he said / she said” conflict, preserves context, and allows professional follow-up. This intersects strongly with patient experience and communication training from conflict resolution in medical admin interactive dictionary, patient advocacy essential terms & interactive role-play scenarios, active listening in healthcare terms & interactive scenarios, and medical office telephone etiquette interactive dictionary & examples.
The professional edge is this: you’re not just “using a CRM.” You’re operating a patient continuity engine with accountability.
5: Future-Proofing Your Healthcare Admin Career With CRM Fluency (Automation, AI, and Modern Patient Expectations)
Healthcare admin work is increasingly digital: online intake, automated messaging, portals, telehealth logistics, and cross-system integrations. That shift doesn’t reduce the need for admins—it increases the need for admins who can manage modern workflows without creating patient frustration. CRM fluency is a high-signal skill because it shows you can think in systems, not just tasks.
This is where CRM terms connect directly to future-focused learning across how AI will transform medical administrative assistant roles by 2030, 10 emerging technologies every CMAA must prepare for in 2025, why automation is the biggest opportunity for CMAA career growth, and interactive guide the medical office of 2025 technologies CMAAs must master.
Here’s what employers increasingly look for in CRM-savvy admin professionals:
You understand data hygiene (clean records = fewer errors).
You can run queues and SLAs (work doesn’t disappear).
You respect consent and privacy boundaries (risk control).
You can build or follow automation rules (scale without chaos).
You can interpret dashboards and KPIs (measure what matters).
Those are the same competence signals described in top 10 skills employers look for in a CMAA, CMAA career roadmap from entry-level to medical office manager, future-proof your CMAA career emerging skills for the next decade, and medical admin assistant job market outlook key trends for 2026-27.
CRM literacy also strengthens exam readiness and real-world performance because it improves your operational vocabulary—how systems talk, how tasks flow, how follow-up happens. That complements certification prep resources like ultimate guide to passing your CMAA certification exam on the first try, interactive CMAA practice exam test your knowledge before exam day, essential study tips to guarantee your CMAA exam success, and complete breakdown what’s included in the 2026-27 CMAA exam.
In plain terms: as healthcare becomes more automated, the winners will be professionals who can keep the patient experience organized, compliant, and human across systems. CRM terms are the language of that future.
6: FAQs: Healthcare CRM Terms, Workflows, and Real Admin Use
-
An EMR is primarily a clinical documentation and patient record system. A CRM focuses on relationship workflows: communications, tasks, pipelines, outreach, referrals, and service cases. Many organizations integrate both to reduce double entry and patient confusion—an area tied to EMR software terms interactive dictionary & walkthroughs, patient management systems interactive dictionary & examples, the future of EMR systems what CMAAs need to know now, and medical office automation trends opportunities for CMAAs.
-
Pipelines, stages, triggers, drip sequences, and consent management. Together, they ensure patients receive the right reminders, intake links, and prep instructions at the right time, and staff can see exactly who is at risk of dropping. This works best when paired with strong scheduling operations from scheduling software glossary interactive guide & tutorials, patient flow management terms interactive guide & scenarios, medical office telephone etiquette interactive dictionary & examples, and active listening in healthcare terms & interactive scenarios.
-
Because tasks without ownership, due times, or escalation rules become invisible. The fix is queue-based monitoring + SLA standards + clear disposition outcomes. This operational maturity overlaps with the broader admin performance themes in new study how certified medical administrative assistants improve healthcare efficiency, medical administration workforce trends key findings for 2025, virtual medical administration how remote work is transforming the role, and how CMAAs will lead the patient experience revolution by 2030.
-
It means tracking a referral from receipt to scheduling to completion and updating the referring source on outcomes/status. It prevents referral drop-offs and builds referrer trust, which is a growth engine for specialty clinics. This ties directly to career growth thinking in CMAA career roadmap from entry-level to medical office manager, future-proof your CMAA career emerging skills for the next decade, interactive career planner future healthcare roles for CMAAs, and annual CMAA job market report where demand is highest.
-
Track opt-in status (especially for SMS), preferred channel, authorized contacts, and any restrictions. Then ensure automation rules respect those settings. This is core to compliance readiness discussed in predicting HIPAA updates & how they will impact CMAAs, CMAAs & data privacy future regulations explained clearly, future healthcare compliance changes how CMAAs can prepare now, and telehealth regulation changes essential insights for CMAAs.
-
Use outcome language: “I understand pipelines and SLAs because I focus on reducing patient leakage—fewer missed callbacks, faster time-to-schedule, and cleaner follow-up documentation.” Then tie it to patient experience skills like clarity, de-escalation, and organized communication using top 10 skills employers look for in a CMAA, medical office telephone etiquette interactive dictionary & examples, conflict resolution in medical admin interactive dictionary, and patient advocacy essential terms & interactive role-play scenarios.