Top 20 Scheduling & Appointment Terms CMAAs Should Know by Heart
In most medical offices, scheduling problems do not begin with the calendar. They begin with misunderstood terms, loose workflows, and front-desk decisions made too fast under pressure. A Certified Medical Administrative Assistant who understands appointment language at a deep operational level can prevent double-booking, reduce no-shows, protect provider time, and keep patients from slipping into frustration before the visit even starts.
This is why scheduling vocabulary is not “basic admin knowledge.” It is operational control. When you know exactly how terms like templating, triage scheduling, lead time, utilization, and referral authorization work inside a real clinic, you stop reacting to chaos and start managing flow with confidence. That same clarity also strengthens your performance in patient intake procedures, improves effective patient communication, supports insurance verification, and helps you adapt to the medical office of 2025.
1. Why Scheduling Terminology Is a Career-Level Skill, Not Just Front-Desk Vocabulary
Scheduling errors can quietly damage every part of a practice. A wrong appointment type creates the wrong time allocation. A missed authorization creates a denied visit. A poorly triaged same-day slot pushes a provider behind for hours. A weak reminder process increases no-shows, which affects revenue, patient trust, and the day’s workflow. This is why strong CMAAs study scheduling language with the same seriousness they bring to healthcare portal terms, telehealth platforms, healthcare CRM terms, and future healthcare compliance changes.
When patients call, they do not describe their needs in scheduling language. They speak in symptoms, worries, urgency, and incomplete information. The CMAA has to translate that messy input into a correct slot, correct provider, correct visit type, correct prep instruction, and correct documentation trail. That translation is impossible without strong command of terms. It also overlaps with the precision needed in medical terminology for medical scribes, the judgment needed for de-escalation techniques, the empathy required in healthcare administration, and the communication discipline that supports medical administrative assistant career growth.
A high-performing CMAA does not merely “book appointments.” They protect access, preserve throughput, prevent avoidable friction, and keep the clinic from bleeding time in five-minute increments all day long.
| Scheduling Breakpoint | What the CMAA Must Confirm | Why It Matters Operationally |
|---|---|---|
| New patient request | Provider acceptance, visit length, intake forms | Prevents wrong-slot booking and registration delays |
| Established patient follow-up | Interval, diagnosis context, needed labs or imaging | Keeps clinical follow-up aligned with care plan |
| Same-day urgent request | Symptoms, escalation pathway, open acute slots | Protects safety and reduces unsafe overbooking |
| Routine physical | Annual eligibility, fasting instructions, paperwork | Avoids patient confusion and claim issues |
| Procedure scheduling | Prep, equipment, room time, consent steps | Prevents downstream delays and cancellations |
| Referral-based visit | Referral status, records, authorization window | Stops revenue leakage and incomplete visits |
| Telehealth appointment | Platform access, patient location, tech readiness | Reduces failed virtual visits |
| Double-book request | Clinical appropriateness, provider approval, buffer impact | Prevents schedule collapse later in the day |
| Waitlist entry | Date range flexibility, preferred times, contact rules | Improves fill rate for canceled slots |
| Reschedule request | Reason, urgency, continuity needs | Protects follow-up compliance |
| Cancellation | Reason, policy, next-step plan | Creates useful data and recovery action |
| No-show review | Reminder history, barriers, policy notes | Supports no-show reduction strategy |
| Provider template block | Admin time, lunch, meetings, procedures | Prevents accidental exposure of protected time |
| Buffer slot | Placement and intended use | Absorbs delays without full schedule drift |
| Lead time check | How far out routine access extends | Reveals access problems early |
| Appointment confirmation | Date, time, provider, location, prep | Cuts avoidable front-desk friction |
| Reminder workflow | SMS, call, email, portal timing | Reduces forgetfulness-related no-shows |
| Arrival window | Early arrival instructions and check-in needs | Protects registration and rooming pace |
| Late patient policy | Minutes threshold and provider discretion | Creates fair and consistent decisions |
| Pre-visit documentation | Forms, ID, insurance card, portal completion | Shortens check-in bottlenecks |
| Visit type conversion | Whether complaint fits booked slot | Prevents mismatch between patient need and schedule design |
| Recall scheduling | Future follow-up cadence by provider protocol | Improves retention and preventive care compliance |
| Cross-location booking | Correct site, provider privileges, patient travel ability | Avoids wrong-location errors |
| Interpreter need | Language support at booking stage | Protects access and visit readiness |
| Insurance-linked appointment type | Coverage rules and visit eligibility | Prevents front-end denial problems |
| Post-procedure follow-up | Timing, symptoms to watch, continuity provider | Reduces missed recovery checks |
| Template optimization review | Utilization, delays, overbook frequency | Supports smarter capacity design |
2. The 20 Scheduling and Appointment Terms CMAAs Should Know by Heart
Below are the 20 terms that separate reactive schedulers from true operational professionals. Mastering them improves your decisions in live calls, portal requests, reminder workflows, and escalation moments. It also strengthens your understanding of HIPAA-related privacy changes for CMAAs, supports cleaner digital workflows in portal communication, and prepares you for technology-driven changes in EMR systems and automation opportunities.
1. Appointment Type
The category of visit being scheduled, such as new patient, follow-up, annual exam, procedure, or telehealth. This term matters because every appointment type drives time length, prep, staffing, documentation expectations, and sometimes billing rules.
2. Provider Template
The structured scheduling grid that defines what kinds of slots are available, when, and for how long. A CMAA must understand the template as a clinical operations tool, not a simple calendar.
3. Slot Length
The amount of time assigned to a visit. Ten extra minutes may be the difference between an orderly clinic and a day that runs behind from the first hour onward.
4. Overbooking
Adding more patients than the designed capacity of a schedule. Sometimes necessary, often dangerous, always something that should be intentional rather than casual.
5. Double-Booking
Placing two patients in the same time block, usually based on provider preference or expected variation in visit demand. It requires judgment, not desperation.
6. Buffer Time
Protected time inserted between visits, procedures, or administrative blocks to absorb delays. Without buffer time, the schedule looks efficient on paper and fails in real life.
7. Lead Time
The number of days between the booking date and the appointment date. Long lead times may signal access problems, patient leakage, or insufficient provider capacity.
8. Triage Scheduling
Prioritizing appointments based on urgency, symptoms, or risk instead of first-come availability alone. This is where scheduling and patient safety intersect.
9. Same-Day Access
Reserved or flexible capacity for urgent but non-emergency needs. Clinics that manage this well reduce frustration, leakage to outside urgent care, and unsafe wait times.
10. Waitlist
A structured list of patients willing to take earlier openings if cancellations occur. A useful waitlist is specific, maintained, and actively worked.
11. Cancellation
A patient or clinic-initiated removal of a scheduled visit before the appointment time. Good offices track cancellation reasons because patterns reveal fixable workflow problems.
12. No-Show
A patient who does not arrive and does not cancel according to policy. No-shows are not just attendance failures; they are often communication, access, or reminder design failures.
13. Recall Scheduling
Booking or prompting future follow-up based on preventive care, chronic disease monitoring, or provider protocol. This is where continuity and retention get operationalized.
14. Confirmation
Direct verification that the patient understands and intends to keep the appointment. Effective confirmations reduce misunderstandings around date, location, provider, and prep.
15. Check-In Window
The expected time before the visit when patients should arrive for registration, documents, and screening. Weak explanation here causes front-desk pileups.
16. Late Policy
The clinic rule governing what happens when patients arrive after a defined threshold. CMAAs need consistency here to avoid conflict and perceived unfairness.
17. Referral Requirement
A condition in which a patient must have referring-provider documentation before a specialist visit. Scheduling without checking this can create wasted appointments and angry patients.
18. Prior Authorization
Approval required by a payer before certain services or visits. This term overlaps directly with insurance verification workflows and affects whether a visit can proceed cleanly.
19. Pre-Visit Prep
Any instructions the patient must complete before the appointment, such as fasting, forms, medications, arrival timing, or uploading records. Missing prep creates avoidable rework.
20. Utilization Rate
How fully available appointment capacity is being used. This metric helps clinics measure access, waste, and whether schedule design matches actual demand.
3. How Strong CMAAs Use These Terms to Prevent Daily Scheduling Failures
Knowing terms is not enough. You need to use them in decision-making. Suppose a patient says they need “a quick appointment” because their medication “isn’t working right.” A weak scheduler hears “quick.” A strong CMAA hears possible symptom escalation, medication management, likely need for triage scheduling, possible need for chart review, and possible mismatch with a standard follow-up slot. That difference protects patients and providers alike. The same decision-making discipline appears in career pathways for medical scribes, essential employer skills, telehealth role evolution, and compliance preparation.
Another common pain point is the appointment that looked correct when booked but fails on the day of service. This usually traces back to one of five front-end misses: the wrong appointment type, unverified insurance, missing referral, absent prep instructions, or poor confirmation. Strong CMAAs think several moves ahead. They do not just ask for the desired date and time. They pressure-test the visit. What is this really for? Is this a routine follow-up or a more complex complaint? Does this provider normally handle it? Is special documentation needed? Has the patient been seen before? Do they need a portal setup step? Is telehealth appropriate? Those questions reduce rework and align closely with skills developed in healthcare documentation trends, real-time healthcare administration insights, AI-driven workflow adaptation, and interactive career planning for CMAAs.
A mature scheduling mindset also respects the emotional temperature of the patient. Patients who are confused, rushed, embarrassed, or already upset will often give incomplete information. If the CMAA is too transactional, the schedule becomes inaccurate. If the CMAA is precise but calm, the patient gives better information and the booking improves. That is where operational skill and patient trust meet.
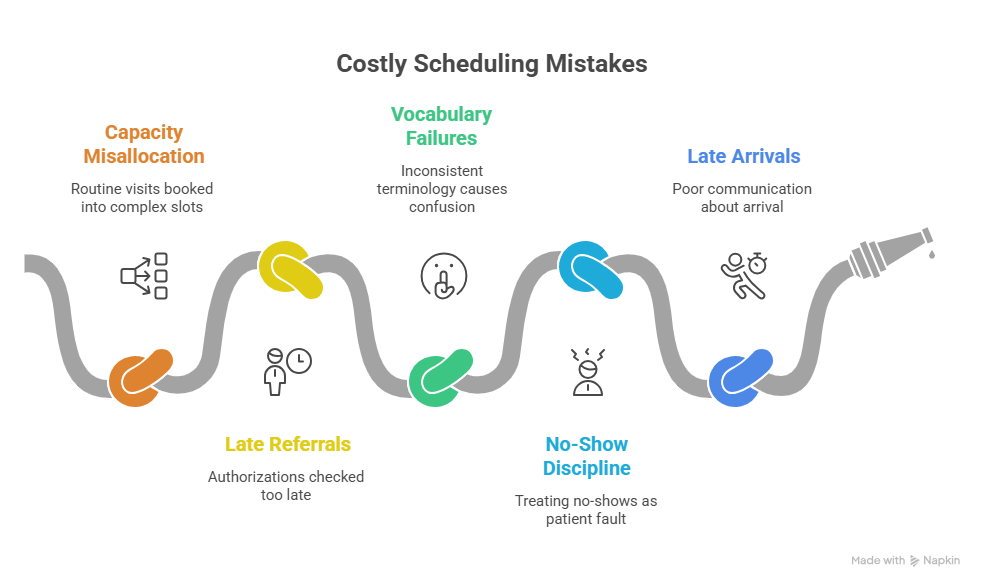
4. The Hidden Scheduling Mistakes That Hurt Access, Revenue, and Patient Trust
The most expensive scheduling mistakes are not dramatic. They are repeated. A clinic loses capacity when routine visits are booked into high-complexity slots and complex needs are squeezed into routine follow-ups. It loses revenue when referrals and authorizations are checked too late. It loses patient trust when the call center promises one thing, the portal says another, and the front desk explains a third. These are vocabulary failures disguised as workflow failures. Teams that strengthen terminology also strengthen medical administration technology readiness, telehealth regulation awareness, data privacy preparation, and major regulatory change planning.
Another hidden mistake is treating every no-show as a patient discipline problem. Many no-shows are built upstream through vague reminders, poor access, confusing prep, bad digital instructions, or failure to explain the importance of the follow-up. When offices study cancellation and no-show reasons by appointment type, they often find preventable patterns. That is why scheduling vocabulary must connect with systems thinking. “Confirmation” is not a box to check. It is a process design question. “Waitlist” is not just a list of names. It is a capacity recovery tool. “Buffer time” is not wasted time. It is protection against cascading failure.
The same applies to late arrivals. If a patient was never told clearly when to arrive, what to bring, how long paperwork might take, or whether portal check-in can reduce time onsite, then the late arrival is partly a communication problem. Strong CMAAs reduce these failures by speaking in operationally meaningful language and making every instruction harder to misinterpret.
5. How to Build Scheduling Mastery That Employers Notice Immediately
If you want this knowledge to become a visible career advantage, study these terms in context rather than as definitions alone. Build mini-scenarios around them. For example: when is overbooking justified? What kinds of visits need built-in buffer? Which specialty visits commonly fail because of missing prep? When should a patient be redirected from a routine slot to triage review? These scenario habits turn vocabulary into judgment. That kind of judgment is exactly what supports long-term value in future-proof CMAA specializations, top emerging career specializations, patient experience leadership, and automation-driven role growth.
A second strategy is to audit your own language. Do you say “What kind of appointment do you want?” or do you guide the patient with focused questions that clarify the actual need? Do you confirm only the date and time, or also provider, location, arrival expectations, and required prep? Do you capture cancellation reasons in a way that can later improve scheduling policy? Employers notice the CMAA who prevents errors before they appear in the queue, not just the one who answers calls quickly.
Finally, connect scheduling knowledge to tools. Learn how templates, reminders, portal workflows, telehealth links, insurance flags, and patient communication fields interact inside real systems. The future belongs to administrative professionals who can combine human judgment with digital workflow fluency. Scheduling mastery is one of the clearest ways to demonstrate that combination.
6. FAQs About Scheduling and Appointment Terms for CMAAs
-
Appointment type is the best starting point because it affects almost everything else: slot length, provider fit, prep, resource needs, and patient expectations. If the appointment type is wrong, the rest of the workflow often fails even if everything else is done correctly.
-
Because overbooking has ripple effects beyond the single slot. It changes wait times, room flow, staff pacing, patient mood, and end-of-day delay. A provider may tolerate it clinically, but the CMAA must still understand its operational cost.
-
Regular scheduling matches a patient to open capacity. Triage scheduling matches the patient to urgency and risk first, then finds the safest appropriate path. It is less about convenience and more about prioritization.
-
Treating them as isolated events instead of data. When cancellation reasons are tracked well, clinics can spot patterns such as long lead times, confusing instructions, transportation barriers, or poor reminder timing.
-
Because apparent productivity and real productivity are not the same. A schedule with no recovery space may look full but can collapse under minor delays. Buffer time helps preserve throughput across the full day instead of maximizing only the early morning hours.
-
At minimum: date, time, provider, location, visit type, arrival expectations, and any required prep. If relevant, also confirm referral status, insurance requirements, portal instructions, and whether the patient has transportation or technology barriers.
-
Use clear, respectful confirmation language that explains practical consequences and preparation steps. Patients are more likely to keep appointments when they understand exactly what is scheduled, why it matters, and what they need to do next.