Patient Privacy Communication Essentials: HIPAA Guidelines Simplified
Patient privacy problems in medical offices rarely begin with dramatic misconduct. They usually begin with rushed habits: a name spoken too loudly, a voicemail that shares too much, a portal message sent without enough thought, a family member answered too casually, a chart discussed where others can hear, or a front-desk explanation that forgets the line between helpful and excessive. HIPAA was built to put structure around those moments by setting national standards for protected health information and how covered entities handle it.
For medical administrative assistants, that makes privacy communication a daily operational skill, not a legal side topic. The goal is not to become a lawyer. The goal is to communicate clearly, verify appropriately, protect trust, and avoid preventable disclosures while keeping the patient experience human. That is why mastering privacy communication belongs right beside front desk operations terms, effective patient communication terms, de-escalation techniques, and top 20 HIPAA & patient privacy terms for medical administrative assistants.
1. What HIPAA Really Means for Everyday Patient Communication
HIPAA is often treated like a scary word people use to shut down conversation. In reality, the HIPAA Privacy Rule creates national standards to protect medical records and other individually identifiable health information, while also allowing appropriate communication for treatment, payment, healthcare operations, and patient rights. It applies to health plans, healthcare clearinghouses, and covered healthcare providers that conduct certain electronic transactions.
For medical admin staff, the most important point is this: privacy communication is not just about whether you can speak. It is about what you say, how much you say, who you say it to, where you say it, and whether you have taken reasonable steps to protect the information. HHS guidance repeatedly emphasizes “reasonable safeguards,” “minimum necessary,” patient rights, and verification of identity or authority where applicable. That means a front-desk worker does not need to freeze at every privacy question. They need disciplined judgment.
That judgment becomes essential because administrative staff often sit at the highest-risk point in the communication chain. They answer incoming calls, verify demographics, discuss scheduling, handle portal questions, route messages, explain paperwork, respond to family members, coordinate referrals, and manage record-access requests. If those actions are loose, privacy breaks down in small ways that can damage trust fast. That is why this topic should be studied alongside patient intake procedures, appointment scheduling best practices, healthcare portal terms, and insurance verification definitions.
The biggest misunderstanding is believing HIPAA forbids communication. It does not. HIPAA supports necessary communication, but it expects covered entities to protect privacy while doing it. That includes using notices of privacy practices, limiting information when the minimum necessary rule applies, and taking reasonable steps to verify identity before disclosing protected health information in situations that require it.
2. The Communication Habits That Prevent Most Front-Desk Privacy Mistakes
The first protective habit is verification without friction. HHS says covered entities must take reasonable steps to verify the identity of a person requesting access or disclosure when required, but those steps should not become barriers that unreasonably delay the patient’s rights. In practice, that means offices need a standard method. Not a random one. If every staff member improvises verification differently, mistakes become inevitable. That is why medical admin teams should connect privacy training to healthcare portal terms, healthcare CRM terms, future healthcare compliance changes, and predicting HIPAA updates.
The second habit is saying less, not because the office is cold, but because precision protects everyone. The minimum necessary requirement means protected health information should not be used, disclosed, or requested when it is not necessary for the purpose, and HHS notes that the entire medical record should not be used or disclosed unless specifically justified when the standard applies. For communication, that means staff should answer the operational question without turning every exchange into an unfiltered information dump.
The third habit is understanding that oral communication counts. HIPAA protections apply to protected health information in oral, written, and electronic forms. That matters because many privacy failures happen in spoken communication, where staff feel informal and therefore less cautious. A low voice, a shorter explanation, a move away from the waiting room, or a decision to continue the conversation through a safer channel can make the difference between competent communication and needless exposure.
The fourth habit is using the office’s Notice of Privacy Practices as a working tool, not a dead handout. HHS says covered healthcare providers generally must develop and distribute a notice explaining privacy practices and patients’ rights. If a patient asks who can see their information, how their records may be shared, or how to obtain a copy, the notice is part of the answer. Strong admin staff know how to explain it in plain language rather than pointing vaguely to paperwork.
3. How to Handle Calls, Messages, Family Questions, and Patient Requests Without Overstepping
Phone communication is where many medical admin assistants feel trapped. The caller wants immediate answers. The office is busy. The tone is urgent. That pressure leads people to over-disclose. The safer approach is structured: verify first, identify the purpose, answer only what is needed, and escalate when the request goes beyond your role. HHS specifically notes that providers may communicate with family, friends, or others involved in the patient’s care or payment in certain circumstances, including by phone, when the patient is present and does not object or when professional judgment supports the disclosure under the rule.
That does not mean every relative who sounds confident should get information. This is a common front-desk pain point. A spouse, parent, adult child, or roommate may expect easy access, and staff under pressure sometimes assume relationship equals authorization. That is risky. The office needs a consistent process for checking whether the patient has involved that person, whether the communication fits care or payment involvement, and whether the information shared is proportionate. Connect that mindset with empathy in healthcare administration, effective patient communication terms, de-escalation techniques, and top 20 scheduling & appointment terms CMAAs should know by heart. Good privacy communication still needs calm language.
Email and similar electronic communications are also permitted under HIPAA when reasonable safeguards are used. HHS explicitly says the Privacy Rule allows providers to communicate electronically with patients, including by email, provided reasonable safeguards are applied, such as checking the email address for accuracy and taking precautions against unintended disclosures. That means the real question is not “Can we email?” but “What is our safe process for emailing?” Offices that do not define that process end up with staff making judgment calls under pressure.
Patient access requests are another major communication test. HHS says individuals have rights to access their protected health information, and covered entities generally must provide access in the form and format requested if it is readily producible, including electronic copies in many circumstances. This is where many offices create frustration by becoming overly defensive. The better approach is privacy with clarity: verify reasonably, explain the process, avoid unnecessary delay, and help the patient understand what comes next.
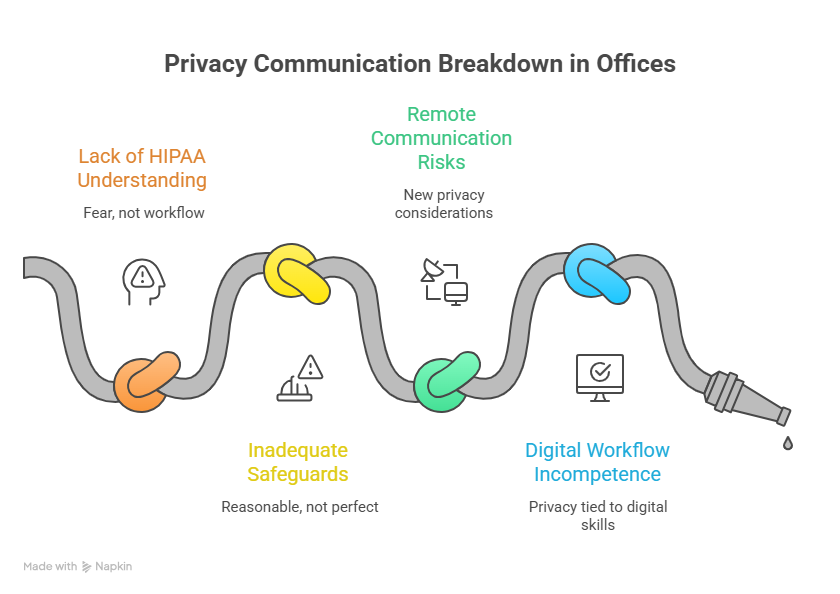
4. The Hidden Places Privacy Communication Breaks Down
Many offices think privacy risk lives only in records release or dramatic breach scenarios. In real life, privacy communication breaks down in ordinary workflows. A patient is called from the waiting room with extra identifying detail. A sensitive diagnosis is left on voicemail. Staff discuss a chart near the check-in window. A portal response includes more clinical content than needed. A caller is “probably the spouse,” so the conversation continues. These failures happen because staff know HIPAA as a fear word rather than an operational workflow.
HHS guidance on incidental disclosures is important here. It explains that certain incidental uses and disclosures may occur as a by-product of an otherwise permitted use or disclosure, as long as reasonable safeguards and minimum necessary policies are in place where applicable. That is a critical nuance. HIPAA does not demand perfection or silence. It demands reasonable safeguards. So the office should ask: Are we lowering voices? Are sign-in or waiting-room processes designed thoughtfully? Are screens and conversations positioned sensibly? Are staff trained to continue sensitive parts of conversations more privately when needed?
Remote communication adds another layer. HHS guidance on telehealth and remote communication highlights privacy and security considerations, including educating patients about protections and using appropriate technologies and safeguards. For admin teams, that means privacy communication now includes phone triage, portal support, appointment setup, remote reminders, and digital follow-up. Medical offices that still think privacy only matters at the filing cabinet are already behind.
This is why future-ready privacy practice should be studied with telehealth platform definitions, virtual medical administration, medical office automation trends, and CMAAs & data privacy future regulations explained clearly. Privacy communication is now tied to digital workflow competence.
5. How Medical Admin Assistants Can Build a Privacy-Safe Communication Style
The strongest privacy-safe communication style is calm, short, verified, and policy-driven. It does not sound robotic, but it does sound consistent. It avoids improvising on sensitive topics. It gives the patient a clear next step instead of a rushed explanation. It understands that being helpful and being private are not opposites.
Start with scripts, but do not stop at scripts. Staff need practical phrases for identity checks, family questions, access requests, portal support, voicemail limits, and escalation points. Then they need to understand why those phrases exist. HHS materials make the structure clear: patients have privacy rights, covered entities need notices of privacy practices, reasonable safeguards matter, the minimum necessary standard matters where applicable, and access rights must be respected. When staff understand those anchors, they communicate with more confidence and less panic.
The next step is linking privacy communication to office outcomes. A privacy-safe office usually also has better intake discipline, cleaner message routing, less rework, stronger patient trust, and fewer emotionally charged confrontations. Patients do not get angry only because of rules. They get angry when the office sounds confused, inconsistent, or evasive. Good privacy communication sounds clear and competent. That is why this topic pairs naturally with how to master medical administrative terminology for your CMAA exam, essential study tips to guarantee your CMAA exam success, future-proof your CMAA career: emerging skills for the next decade, and interactive guide: the medical office of 2025 technologies CMAAs must master.
Finally, offices should treat privacy communication as retrainable. If the team keeps stumbling over family calls, voicemail wording, or portal messaging, that is not proof HIPAA is “too complicated.” It is proof the workflow needs training, scripting, and reinforcement. Privacy should not live as a once-a-year compliance slideshow. It should live inside daily communication habits.
6. FAQs
-
No. HHS says providers may communicate electronically, including by email, with patients if they apply reasonable safeguards, and phone communication is also permitted when handled appropriately.
-
Usually it is over-disclosure under pressure: sharing too much on a call, voicemail, or desk conversation because the staff member is trying to be helpful quickly rather than precisely.
-
Sometimes. HHS guidance says providers may communicate with family, friends, or others involved in the patient’s care or payment in certain circumstances, especially where the patient is present and does not object or where the rule otherwise permits it.
-
It means when the rule applies, the office should use, disclose, or request only the information reasonably needed for the purpose, not everything available.
-
Not automatically. HHS recognizes some incidental disclosures can occur if the main use or disclosure is permitted and reasonable safeguards are in place.
-
Yes. HHS says covered entities should take reasonable steps to verify identity or authority when required, but those steps should not create unreasonable barriers to access.
-
Yes. HHS says individuals have a right to access protected health information, including in requested forms and formats when readily producible.