Predictive Analytics in Medical Administration: Opportunities & Skills Needed
Predictive analytics is starting to reshape medical administration in the same way scheduling software, EMRs, and patient portals once did. The difference is that it does not just organize work after the fact. It helps offices anticipate no-shows, staffing strain, payer delays, scheduling bottlenecks, patient communication breakdowns, and revenue leakage before those problems become expensive.
That creates a major opportunity for medical admin professionals. The people who understand operations and can work confidently with data, workflows, and digital tools will become far more valuable than those who only execute repetitive tasks. This guide explains where predictive analytics matters most, what opportunities it creates, and which skills medical admin professionals need to stay relevant.
1. Why Predictive Analytics Matters in Medical Administration Right Now
Medical administration has always involved prediction, even when offices did not call it that. Front-desk staff learned to anticipate which time blocks would run late. Schedulers noticed which patients were likely to no-show. Revenue teams recognized patterns in denials. Supervisors learned when call volume would spike, when staffing gaps would hurt access, and when documentation issues would slow reimbursement. Predictive analytics turns those instincts into a more structured, measurable, and scalable capability.
That matters because modern medical offices are under pressure from every direction. Patient expectations are higher. Staffing is thinner. Administrative waste is harder to hide. Providers want fewer interruptions. Leadership wants better access, cleaner workflows, faster collections, and stronger patient retention. A medical admin professional who understands medical office automation trends, AI and automation in medical administration, interactive emerging medical admin technologies, virtual medical administration, and future-proofing your CMAA career is already better positioned to explain why prediction-based workflows matter.
In practice, predictive analytics helps healthcare teams act earlier. Instead of reacting after the schedule falls apart, offices can identify high-risk appointment slots, chronic no-show patterns, insurance verification delays, repeat referral bottlenecks, and call queue surges. Instead of waiting for patient dissatisfaction to show up in complaints, teams can spot friction points in check-in, portal response times, and appointment lead times. That kind of visibility is especially powerful for administrative staff because so many patient and revenue problems begin in admin workflows, not in the exam room.
There is also a career reason to pay attention. Medical admin roles are changing. Purely repetitive work is becoming easier to automate. Roles built around operational judgment, exception handling, patient communication, workflow analysis, and tool fluency are becoming more valuable. Reading interactive industry report on medical administration job demand by specialty, medical admin assistant job market outlook, new study on how certified medical administrative assistants improve healthcare efficiency, 2026 healthcare administration report, and future-proof your CMAA career with emerging skills makes that shift hard to ignore.
Most importantly, predictive analytics gives medical admin professionals a way to move from task support to operational impact. The person who can explain why no-shows are rising, which patient groups need different reminder strategies, where authorizations get stuck, and how schedule patterns affect access is far more useful than the person who simply processes the same workflow every day without questioning it. That is the real opportunity.
| # | Predictive Use Case | What It Helps Forecast | Admin Value | Skills Needed |
|---|---|---|---|---|
| 1 | No-show risk | Which patients are most likely to miss appointments | Improves fill rates and reminder targeting | Scheduling analysis, outreach logic |
| 2 | Late arrivals | Time blocks likely to run behind | Helps reduce provider bottlenecks | Template awareness, check-in timing |
| 3 | Call surge prediction | Peak call periods by day and season | Improves staffing coverage | Phone metrics review, staff coordination |
| 4 | Portal message volume | High-response windows and backlog risk | Prevents patient communication delays | Inbox triage, digital workflow management |
| 5 | Insurance verification delays | Payers or plans likely to slow registration | Reduces day-of-service friction | Payer literacy, previsit prep |
| 6 | Authorization bottlenecks | Cases likely to stall before service | Protects access and revenue | Referral tracking, payer follow-up |
| 7 | Denial risk | Common admin-driven claim problems | Supports cleaner front-end workflows | Revenue cycle awareness |
| 8 | Referral leakage | Patients unlikely to complete referrals | Improves continuity and downstream revenue | Follow-up discipline, coordination |
| 9 | Cancellation patterns | Specialties or slots with repeat cancellations | Strengthens template design | Schedule optimization |
| 10 | Patient churn | Who may stop returning for care | Supports retention strategy | Patient communication analysis |
| 11 | Reschedule likelihood | Appointments likely to shift repeatedly | Improves queue planning | Workflow pattern recognition |
| 12 | Front-desk congestion | Check-in times most prone to backups | Improves staffing and flow | Arrival pattern analysis |
| 13 | Records request volume | Periods with high release-of-information demand | Prevents admin backlog | Records workflow management |
| 14 | Payment collection risk | Balances less likely to be resolved quickly | Supports better follow-up planning | Billing basics, communication timing |
| 15 | Staffing strain | Days or shifts likely to overload teams | Improves coverage decisions | Productivity tracking, workforce planning |
| 16 | Provider schedule drift | Visit types that regularly overrun | Reduces avoidable delays | Template discipline, visit-type review |
| 17 | Patient complaint risk | Touchpoints linked to dissatisfaction | Improves service recovery | Experience analysis, escalation awareness |
| 18 | Portal adoption gaps | Patients unlikely to use digital tools | Improves outreach channel decisions | Patient education, segmentation |
| 19 | Reminder effectiveness | Which outreach methods work by group | Improves attendance and response rates | Communication testing, data review |
| 20 | Registration error risk | Where demographic or insurance errors cluster | Reduces rework and claim issues | Quality control, intake accuracy |
| 21 | EMR task backlog | Teams likely to fall behind on messages or tasks | Protects continuity and responsiveness | Queue monitoring, prioritization |
| 22 | Telehealth no-show risk | Virtual visits likely to fail technically or behaviorally | Improves prep and access support | Digital support workflow |
| 23 | Seasonal volume shifts | Recurring spikes in specific services | Supports smarter staffing and scheduling | Trend analysis, planning cadence |
| 24 | Follow-up compliance risk | Patients least likely to complete next steps | Improves care continuity | Reminder workflow design |
| 25 | Documentation lag | When operational handoffs are likely to slow | Improves timing and accountability | Process mapping, handoff discipline |
| 26 | Access bottlenecks by specialty | Specialties with rising scheduling pressure | Supports capacity planning | Referral and scheduling insight |
| 27 | Patient communication dropout | Messages or reminders likely to go unanswered | Improves outreach strategy | Contact hygiene, channel optimization |
2. The Biggest Opportunities Predictive Analytics Creates for Medical Admin Professionals
The first major opportunity is stronger scheduling performance. Scheduling is one of the most data-rich parts of medical administration, yet many offices still treat it like a reactive task. Predictive tools can flag high-risk no-shows, recurring late arrivals, visit types that regularly cause delays, provider templates that create backlog, and reminder workflows that underperform for certain patient groups. A professional who understands appointment scheduling best practices, the interactive guide to handling scheduling conflicts, emergency appointment management, scheduling software mastery, and medical appointment scheduling tools ranked by ease of use can translate predictions into better real-world scheduling decisions.
The second opportunity is front-end revenue protection. Many revenue problems begin long before a claim is submitted. They start with bad demographics, poor insurance capture, missing authorizations, weak referrals, or inconsistent eligibility checks. Predictive models can help flag which appointments are likely to run into front-end financial friction before the patient reaches the desk. Medical admin professionals who understand insurance verification, top 20 medical billing terms all CMAAs should understand, CPT codes explained, ICD-10 codes interactive dictionary, and patient intake procedures are better equipped to support this work.
The third opportunity is patient communication optimization. Many healthcare offices still send the same reminders, the same portal messages, and the same follow-up wording to everyone. Predictive analytics can show which patient segments respond to text versus call, which groups need earlier reminders, which portal users are likely to ignore messages, and where communication drop-off is most common. That creates a role for admin professionals who understand patient communication apps, effective patient communication, active listening techniques, patient privacy communication essentials, and healthcare portal use cases.
The fourth opportunity is operational leadership. Offices need people who can look at patterns and say something useful: why Mondays are overloaded, why one provider’s clinic always runs behind, why one payer causes repeat rescheduling, why call queues explode after certain reminder campaigns, or why portal response times keep slipping. Predictive analytics makes these patterns easier to detect, but people still need to interpret them. That is where medically literate, workflow-aware admin staff become valuable. Building that perspective through front-desk operations guidance, medical admin time tracking tools, best collaboration tools for medical office teams, directory of staff scheduling tools, and professional organizations for medical admin assistants can elevate your role well beyond daily task execution.
3. Where Predictive Analytics Shows Up First in Real Medical Office Workflows
Predictive analytics often enters medical administration quietly. It may first appear inside scheduling software, patient communication tools, EMR dashboards, reporting modules, call center platforms, or revenue cycle systems. That matters because many professionals assume predictive analytics belongs only to data teams. In reality, admin teams may be using prediction-driven features before they even realize it.
One obvious area is appointment attendance. If a platform helps identify patients who may miss appointments or suggests additional reminders for certain visit types, that is predictive thinking built into workflow. Another area is staffing. If management uses historical patterns to anticipate heavy registration days, portal volume spikes, or call surges, that is operational forecasting. Medical admin professionals who understand secure patient scheduling tools, patient communication apps, EMR integration tools, telehealth platforms, and healthcare CRM terms will notice these patterns sooner.
Another early use case is quality control. Offices can track where intake errors are happening, which forms are most often incomplete, what kinds of records requests create delays, and where patient follow-up gets lost. These are not abstract analytics questions. These are daily medical admin problems. Someone who studies tools for efficient medical records release, interactive training on patient record updates, resolving common EMR software issues, infection control in medical offices, and top 10 EMR shortcuts will usually have a stronger eye for where structured data and workflow discipline meet.
It also shows up in patient access strategy. Predictive models can help offices anticipate referral completion risk, scheduling delays by specialty, patient churn, portal non-adoption, and communication dropout. That means medical admin staff involved in access, follow-up, registration, and patient support are already part of the predictive workflow whether the organization labels it that way or not.
4. The Skills Medical Admin Professionals Need To Work Confidently With Predictive Analytics
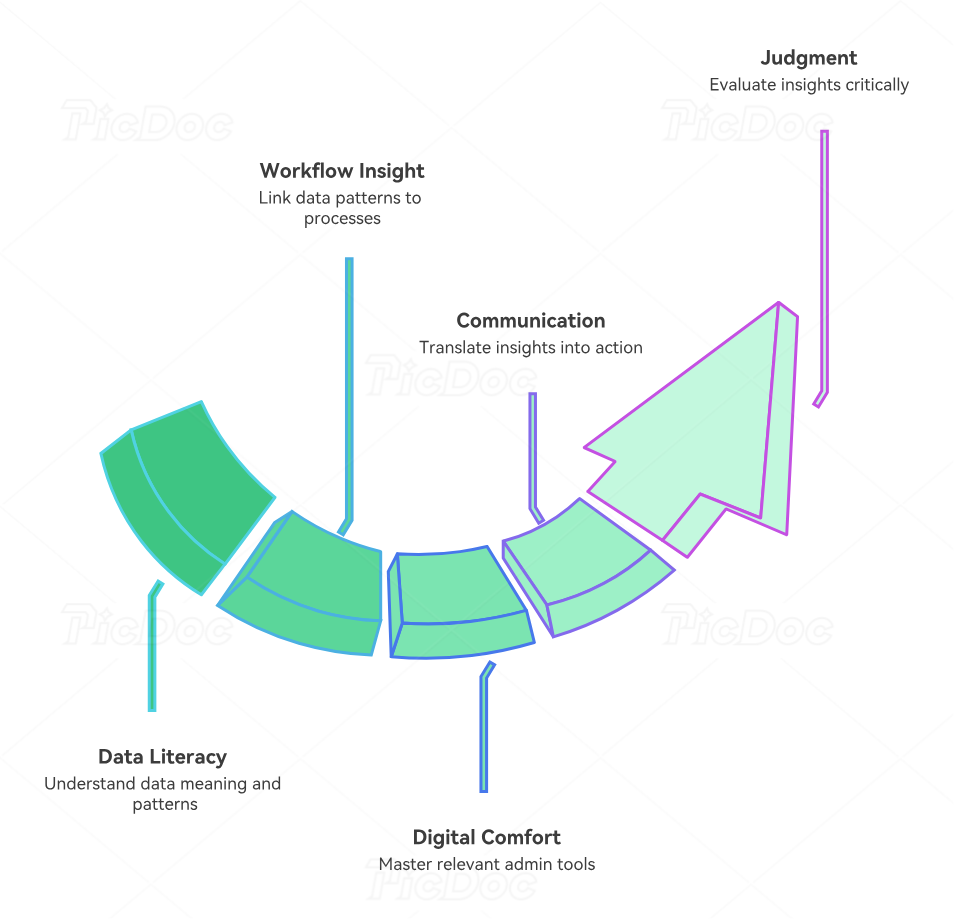
You do not need to become a data scientist to work well with predictive analytics. You do need a stronger skill stack than basic task execution. The first required skill is data literacy. That means understanding what the numbers represent, where they come from, how they can be misleading, and what patterns are worth investigating. If no-show rates spike, you need to ask whether the cause is reminder failure, schedule lead time, transportation issues, patient demographics, specialty type, or inaccurate contact information. Data literacy is really structured curiosity.
The second skill is workflow understanding. Predictive analytics is only useful when someone can connect the pattern to the process. A dashboard may show that one appointment type has higher reschedule rates, but that insight only becomes valuable when an admin professional can link it to template design, patient instructions, authorization timing, or outreach gaps. Deepening your workflow fluency through front-desk operations, patient intake procedures, appointment conflict handling, medical records release tools, and staff scheduling tools makes interpretation much stronger.
The third skill is digital tool comfort. Modern admin work increasingly depends on platforms that combine scheduling, communications, charting, reporting, and patient engagement. Someone intimidated by dashboards, filters, queues, rules, and workflow settings will struggle to benefit from predictive systems. That is why it helps to study EMR integration tools, healthcare portals, telehealth platforms, medical office automation trends, and interactive emerging admin technologies.
The fourth skill is communication. Predictive analytics does not create value until someone turns a pattern into action. You may need to explain to a supervisor why certain reminder workflows are underperforming, to a provider why one clinic template keeps running late, or to teammates why registration quality problems are clustering in one area. That requires concise, non-dramatic communication. Resources like effective patient communication, active listening techniques, best collaboration tools for medical office teams, online communities for CMAAs, and networking strategies for medical admin professionals can sharpen that side of the role.
The fifth skill is judgment. Not every pattern deserves a major workflow change. Small sample sizes can mislead. Seasonal shifts can distort comparisons. One broken process can create bad data. Predictive analytics becomes dangerous when people treat every dashboard insight as truth without checking operational reality. The best medical admin professionals will combine data awareness with grounded skepticism.
5. How To Start Building Predictive Analytics Skills Without Becoming Overwhelmed
The best entry point is not advanced math. It is better observation. Start paying closer attention to patterns in your daily work. Which appointments get canceled most often? Which reminders seem to work poorly? Which providers run behind in predictable ways? Which payer issues keep appearing at check-in? Which days produce the worst call pileups? Which patient instructions create the most confusion? This habit of noticing patterns is the foundation of predictive thinking.
Next, learn to work backward from operational pain points. Predictive analytics is most useful when it solves something painful: no-shows, authorizations, portal delays, front-desk congestion, registration errors, low collections, or follow-up dropout. Once you identify the pain point, ask what signals might predict it earlier. That is how an admin professional starts thinking more strategically.
Then strengthen your terminology and tool fluency. Many people struggle with data-driven work because the surrounding healthcare workflow is still fuzzy to them. You will understand analytics better when you already understand the operation being measured. That is why it helps to keep building fluency through how to master medical administrative terminology for your CMAA exam, complete breakdown of the CMAA exam, top skills employers look for in a CMAA, CMAA career roadmap, and why CMAA certification dramatically boosts career opportunities.
You should also become more comfortable with simple metrics. Learn how to read trend lines, compare periods, spot outliers, and ask better follow-up questions. You do not need advanced modeling to add value. An office gains a lot from someone who can say, “These cancellations are rising fastest in one appointment category,” or “This reminder sequence works poorly for one patient segment,” or “This payer keeps creating verification friction on the front end.”
Finally, position these skills in career terms. On a resume or in an interview, you can frame yourself as someone who improves scheduling performance, strengthens patient communication, reduces rework, supports cleaner workflows, and uses system data to identify operational issues early. That is a much stronger market position than simply calling yourself organized.
6. FAQs
-
It is the use of historical and current data to anticipate operational issues before they become bigger problems. In medical administration, that can include forecasting no-shows, staffing strain, authorization delays, call surges, patient churn, registration errors, or communication drop-off. The goal is earlier action, not just better reporting after the damage is already done.
-
Usually, no. Most medical admin roles benefit more from data literacy, workflow understanding, digital tool comfort, and pattern recognition than from advanced technical modeling. You do need to understand what a metric means, what might distort it, and how to act on it inside a real workflow.
-
Start with scheduling analysis, patient communication workflows, front-end revenue literacy, EMR and portal comfort, and basic trend interpretation. Strong foundations come from appointment scheduling best practices, insurance verification, EMR compliance training, medical admin time tracking tools, and AI and automation in medical administration.
-
Scheduling, reminders, registration quality, authorization tracking, call volume planning, and portal backlog management are often the fastest win areas. These are high-friction admin workflows with lots of measurable activity and clear operational consequences.
-
Talk about pattern-based improvement. Explain how you noticed recurring scheduling bottlenecks, patient communication gaps, registration errors, or workflow delays and how you would use system data to investigate them more formally. That shows predictive thinking even without a formal analytics title.
-
It will replace some repetitive parts of the work and increase the value of higher-judgment roles. The strongest professionals will be the ones who can combine patient communication, workflow knowledge, tool fluency, privacy awareness, and data interpretation. That combination is much harder to automate than repetitive admin execution alone.