How to Become an Expert Pediatric Medical Scribe
Pediatric scribing demands sharper listening, faster context-building, and cleaner clinical judgment support than many entry-level scribes expect. A child may speak, a parent may interpret, and the provider may be weighing age-specific risks in real time. To grow from beginner to expert, you need more than typing speed; you need pediatric vocabulary, visit-flow discipline, EMR confidence, privacy awareness, and documentation habits strong enough for busy clinics, urgent care, and emergency settings. Start by pairing medical scribe certification preparation with pediatric and OB/GYN documentation exposure, EMR charting fluency, and accurate clinical documentation habits.
1. Build the Pediatric Documentation Foundation First
An expert pediatric medical scribe understands that every pediatric note begins with context. Age changes the meaning of symptoms, risk, vital signs, medication history, immunization relevance, and even the reliability of the history. A fever in a teenager, a fever in a toddler, and a fever in a newborn can lead the provider down very different clinical pathways, so your note must preserve age, source of history, timing, exposures, intake, output, behavior changes, and the provider’s clinical reasoning with precision. That is why pediatric scribing should be built on core medical scribe terminology, medical terminology study methods, HPI accuracy standards, and documentation accuracy training.
The first skill to master is historian clarity. Pediatric encounters often include multiple voices: the child, parent, grandparent, foster parent, school nurse note, daycare report, or EMS summary. Your documentation should identify where the history came from and preserve contradictions without making them look like provider uncertainty. A parent may say the child “has not eaten all day,” while the child says they had snacks at school; an expert scribe captures the provider’s clarified timeline instead of turning competing details into a messy HPI. This discipline connects directly to effective patient communication, active listening in medical administration, patient intake procedures, and front-desk operations awareness.
The second skill is pediatric specificity. “Cough” is thin. “Three days of dry cough, worse at night, associated with post-tussive emesis, decreased appetite, normal urine output, sick contacts at daycare, no increased work of breathing reported” gives the provider a usable clinical frame. “Rash” is thin. “Pruritic rash beginning on trunk after new antibiotic exposure, spreading to arms, no mucosal involvement reported, provider notes blanching maculopapular appearance” is far more defensible. That level of note quality is exactly where specialty-specific documentation templates, ICD-10 code awareness, CPT reference knowledge, and EMR platform familiarity become practical tools.
| # | Pediatric Scribe Skill | Why It Matters in Real Encounters | Expert-Level Documentation Move |
|---|---|---|---|
| 1 | Age-specific chief complaint framing | Symptoms carry different urgency based on age and development stage. | Lead the HPI with age, symptom duration, caregiver source, and provider-confirmed context. |
| 2 | Historian identification | Parents, guardians, teens, school notes, and EMS reports can conflict. | Document “history provided by mother/father/guardian/patient” when clinically relevant. |
| 3 | Fever documentation | Temperature source, height, duration, and medication response influence provider reasoning. | Capture measured temperature, route, antipyretic timing, associated symptoms, and provider assessment. |
| 4 | Feeding history | Feeding changes can signal dehydration, respiratory effort, pain, or systemic illness. | Specify breast/formula/solids intake, change from baseline, vomiting, and tolerance. |
| 5 | Urine output tracking | Wet diapers and voiding frequency often matter more than vague “drinking less.” | Chart exact caregiver-reported wet diapers, last urination, and provider interpretation. |
| 6 | Immunization awareness | Vaccine status affects differential thinking, counseling, and school documentation. | Record “up to date,” delayed, unknown, or specific missing vaccines only as confirmed. |
| 7 | Medication dose clarity | Pediatric dosing depends on weight, concentration, and timing. | Capture medication name, concentration when stated, dose, route, frequency, and last dose. |
| 8 | Allergy precision | True allergies, side effects, and family concerns may be mixed together. | Separate medication allergy, food allergy, reaction type, severity, and provider clarification. |
| 9 | Developmental milestone awareness | Delay, regression, or age-inappropriate behavior can change the visit direction. | Document provider-noted milestones, regression concerns, school performance, and referrals. |
| 10 | Growth chart context | Weight, height, BMI, and head circumference affect longitudinal pediatric care. | Record provider interpretation of trend concerns rather than inventing significance. |
| 11 | Respiratory distress language | Retractions, nasal flaring, wheeze, stridor, and work of breathing carry high acuity. | Use provider-stated exam terms and avoid softening urgent respiratory findings. |
| 12 | Rash description discipline | Distribution, appearance, blanching, mucosal involvement, and exposure history matter. | Capture morphology only when provider describes or confirms it. |
| 13 | Ear pain and otitis workflow | Ear complaints often need laterality, fever, URI symptoms, and exam precision. | Document right/left/bilateral findings, tympanic membrane language, and treatment plan. |
| 14 | Asthma and wheezing history | Triggers, inhaler use, hospitalizations, and steroid history guide risk. | Include controller/rescue medication use, last treatment, nighttime symptoms, and provider plan. |
| 15 | Sports injury detail | Mechanism, location, neurovascular status, and return-to-play guidance matter. | Chart mechanism, exam, imaging plan, restrictions, and follow-up instructions. |
| 16 | Abdominal pain timeline | Migration, vomiting, stool changes, urinary symptoms, and appetite affect workup. | Preserve onset, location, progression, associated symptoms, and provider differential language. |
| 17 | Adolescent confidentiality awareness | Teen visits may include sensitive history, private discussion, and guarded documentation. | Follow provider workflow and clinic policy for confidential portions of the note. |
| 18 | Behavioral health documentation care | Depression, anxiety, self-harm screening, and school stress require exact phrasing. | Capture screening results, safety statements, referrals, and follow-up plan accurately. |
| 19 | Safeguarding red-flag awareness | Injury patterns, delayed care, and inconsistent stories require careful provider documentation. | Record observed findings and provider statements without emotional wording. |
| 20 | School and daycare exposure history | Contagion, outbreaks, sick contacts, and return notes often drive pediatric visits. | Capture exposure setting, symptom clusters, and provider return-to-school guidance. |
| 21 | Procedure documentation | Wound care, splinting, strep swabs, vaccines, and nebulizer treatments require traceable notes. | Include indication, consent when stated, provider performer, tolerance, and aftercare. |
| 22 | Patient education capture | Pediatric plans rely heavily on caregiver instructions and warning signs. | Document hydration advice, medication instructions, return precautions, and follow-up timing. |
| 23 | EMR template control | Templates save time while also creating copy-forward risk. | Use EMR platform knowledge to clean irrelevant defaults before provider review. |
| 24 | HIPAA awareness | Parents, guardians, minors, and teen privacy create complex information boundaries. | Support provider workflow through HIPAA terminology fluency and careful chart access habits. |
| 25 | Care plan sequencing | Families need clear next steps, medications, labs, imaging, and follow-up. | Use plan bullets in the order the provider communicates them. |
| 26 | Return precaution accuracy | Caregivers rely on specific danger signs after leaving the clinic. | Preserve provider-stated red flags, timing, and escalation instructions. |
| 27 | Referral tracking | Pediatrics often involves ENT, allergy, pulmonology, GI, ortho, speech, or behavioral health. | Document specialty, reason, urgency, and supporting tests or counseling. |
| 28 | Exam language restraint | Pediatric exam findings require accuracy and provider confirmation. | Use provider-confirmed terminology from scribe exam mistake prevention and real chart review. |
| 29 | Visit closure discipline | A strong pediatric note ends with family understanding and follow-up clarity. | Capture caregiver agreement, questions answered, follow-up interval, and emergency precautions. |
| 30 | Career proof building | Pediatric roles reward scribes who can show specialty readiness. | Pair medical scribe career growth with pediatric-specific examples and training artifacts. |
2. Master the Pediatric HPI, ROS, Exam, and Plan Structure
The pediatric HPI must make the provider’s thinking easy to follow. Start with the child’s age and reason for visit, then build the timeline around onset, severity, progression, modifying factors, associated symptoms, exposure history, home treatment, intake, urine output, behavior, and the family’s main concern. A strong HPI avoids vague filler and preserves medically useful detail. Instead of writing “child is sick,” document fever duration, highest temperature, cough pattern, vomiting episodes, stool changes, daycare exposure, appetite change, medication timing, and provider-confirmed negatives. This is where HPI documentation accuracy, medical terminology mastery, interactive practice exam preparation, and scribe certification exam breakdowns should shape your daily practice.
The pediatric review of systems requires smart listening because caregivers often describe symptoms in everyday language. “Breathing funny” may become provider-confirmed increased work of breathing, wheezing, retractions, congestion, or cough. “Not acting right” may require notes on lethargy, irritability, decreased play, poor feeding, or altered responsiveness if the provider confirms those terms. Your job is to translate the encounter into accurate clinical language while keeping the provider’s wording, certainty level, and logic intact. This skill grows through top EMR and charting terms, real-life scribe questions, ER scribing training, and urgent care scribe job exposure.
The exam section should be clean, restrained, and provider-led. Pediatric exams can move quickly because the provider may observe general appearance, hydration, respiratory effort, ear findings, throat findings, abdominal tenderness, rash distribution, neurologic status, and interaction with caregiver in a short window. Expert scribes resist the temptation to overbuild the exam from assumptions. If the provider says the child is well appearing, interactive, and hydrated, document that. If the provider confirms retractions, abnormal tympanic membrane findings, abdominal guarding, or concerning rash features, preserve those terms exactly. Your accuracy depends on documentation template discipline, EMR shortcut training, common EMR software issue resolution, and patient record update compliance.
The plan section is where many pediatric notes either become useful or become risky. Families need exact medication instructions, weight-based dosing if the provider states it, hydration guidance, school or daycare instructions, return precautions, referral details, test results, and follow-up timing. A pediatric plan should clearly separate treatment, testing, caregiver education, and escalation instructions. “Follow up as needed” often lacks the precision families need; “return for worsening breathing, persistent fever, signs of dehydration, or inability to tolerate fluids, and follow up with pediatrician in 48 hours” carries much more practical value when that is what the provider communicated. Build this habit through patient privacy communication essentials, effective patient communication terms, telehealth platform documentation, and medical scribe skills beyond documentation.
3. Learn Pediatric Workflows by Setting, Specialty, and Visit Type
Pediatric scribing changes by setting. In primary care, expert scribes support preventive visits, growth tracking, vaccine counseling, developmental screening, school forms, medication refills, asthma action plans, ADHD follow-ups, and parent education. These notes require continuity because the provider may compare today’s findings to prior visits, growth trends, school performance, and family concerns. If you want to become valuable in outpatient pediatrics, study primary care and family medicine scribe networks, pediatric and women’s health hiring networks, community health center scribe opportunities, and medical scribe career outlook data.
Urgent care and emergency pediatrics demand faster triage awareness. The provider may focus on respiratory distress, dehydration, fever risk, head injury, abdominal pain, allergic reaction, laceration, fracture, seizure, toxic ingestion, or behavioral health crisis. You must keep pace while preserving time-sensitive details: last oral intake, last wet diaper, last medication dose, mechanism of injury, loss of consciousness, vomiting after head injury, wheezing history, epinephrine use, and response to treatment. Build this pace with emergency room scribing training, urgent care and retail clinic job directories, top emergency departments hiring scribes, and day-in-the-life emergency department scribe stories.
Specialty pediatrics expands your vocabulary and sharpens your template discipline. Pediatric cardiology requires murmur history, exertional symptoms, syncope context, family history, and test tracking. Pediatric orthopedics requires mechanism, laterality, neurovascular status, imaging, bracing, and activity restrictions. Pediatric dermatology requires lesion morphology, distribution, triggers, treatment response, and infection concerns. Pediatric oncology requires careful symptom tracking, medication history, treatment timeline, and provider-led assessment language. You can widen your readiness with cardiology scribe skills, orthopedic scribing training, dermatology and ophthalmology hiring networks, and advanced oncology scribing guidance.
Telehealth pediatrics brings a different pressure point: the provider may depend heavily on caregiver observation, camera-based appearance, reported vitals, photos of rashes, home pulse oximetry, or school/daycare exposure. Your documentation must show what was reported, what was visually assessed, what limitations existed, and what follow-up or escalation the provider recommended. Remote pediatric scribing also requires privacy discipline because minors, parents, siblings, and shared spaces may create sensitive communication issues. Prepare through remote medical scribe market growth, telehealth companies using scribes, remote scribe employer directories, and telehealth platform terminology.
4. Become Reliable Under Pressure Without Losing Accuracy
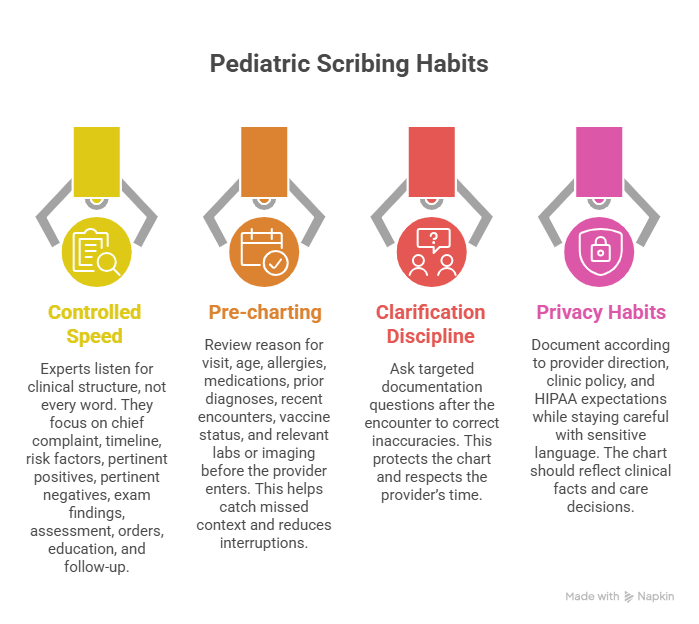
Speed matters in pediatric scribing, but controlled speed matters more. A beginner tries to type every word. An expert listens for the clinical structure of the visit: chief complaint, timeline, risk factors, pertinent positives, pertinent negatives, exam findings, assessment, orders, education, and follow-up. In a busy pediatric shift, the provider may move from ear infection to asthma flare to sports injury to newborn feeding concern within minutes. Your system should help you catch the right details quickly. Develop that system through essential study techniques for certification success, scribe exam mistake prevention, ACMSO exam day essentials, and medical scribe practice exams.
The most useful pressure habit is pre-charting. Before the provider enters, review the reason for visit, age, allergies, medications, prior diagnoses, recent encounters, vaccine status if available, and relevant labs or imaging. In pediatrics, pre-charting helps you catch missed context, such as recurrent otitis media, asthma controller use, prior ED visits, prematurity history, prior specialist referral, or medication allergy. The goal is a cleaner note and fewer provider interruptions. This workflow becomes stronger when paired with EMR integration tool knowledge, medical records release awareness, healthcare portal terminology, and interactive patient record compliance training.
Another expert habit is clarification discipline. Pediatric notes can be damaged by tiny inaccuracies: wrong laterality, vague fever timing, missing last dose, unclear weight-based medication instructions, or confusing suspected diagnosis with confirmed diagnosis. When clinic workflow allows, ask the provider targeted documentation questions after the encounter: “Did you want the rash described as diffuse or localized?” “Should the plan include return precautions for breathing difficulty and dehydration?” “Was the assessment viral URI with wheeze or asthma exacerbation?” Targeted clarification protects the chart and respects the provider’s time. Build that professional judgment through top medical scribe exam mistakes, real-life exam questions, patient communication examples, and de-escalation communication techniques.
Pressure also tests your privacy habits. Pediatric scribes may encounter divorced parents, custody questions, foster care documentation, adolescent sexual health, behavioral health concerns, abuse concerns, school requests, and portal access issues. Your role is to document according to provider direction, clinic policy, and HIPAA expectations while staying careful with sensitive language. The chart should reflect clinical facts, provider statements, and care decisions with clean boundaries. Strengthen this area through HIPAA terms for scribes, patient privacy communication essentials, top HIPAA terms for medical administrative assistants, and empathy in healthcare administration.
5. Turn Pediatric Scribe Skills Into Career Proof
Expertise becomes visible when you can show your training, accuracy, specialty readiness, and professional habits. If you want pediatric clinics, children’s hospitals, urgent care networks, telehealth groups, or pediatric specialty practices to take you seriously, build a small career portfolio around pediatric documentation. Include completed training, EMR practice, sample de-identified note structures, specialty vocabulary lists, and examples of how you handle HPI structure, return precautions, and caregiver education. This pairs naturally with medical scribe certification guidance, medical scribe training courses, how becoming a scribe boosts your medical career, and career outlook insights.
When applying for pediatric scribe roles, speak in outcomes. Hiring managers care about whether you can protect provider time, reduce chart cleanup, support accurate documentation, adapt to specialty workflows, and work professionally around children and families. Replace generic claims like “good with kids” with stronger evidence: “trained in pediatric HPI structure, vaccine-status documentation, caregiver education capture, asthma and URI note patterns, and return-precaution documentation.” This language aligns with why facilities prefer certified medical scribes, medical scribe workforce reports, top hospitals hiring medical scribes, and health systems hiring by state.
You should also learn where pediatric scribe demand appears. Pediatric roles can sit inside children’s hospitals, primary care groups, urgent care chains, telehealth companies, community health centers, academic medical centers, and specialty clinics. A smart job search uses multiple pipelines because pediatric documentation experience may be listed under pediatric medical assistant support, clinical documentation assistant, remote scribe, outpatient scribe, ER scribe, or specialty scribe. Search across top pediatric and OB/GYN networks, academic medical centers using scribes, physician groups and MSOs hiring scribes, and healthcare recruiters posting scribe roles.
Finally, keep improving after you get the role. Track recurring pediatric diagnoses, provider preferences, missed details during chart review, unfamiliar medications, commonly used templates, and return-precaution language. Ask for feedback on your HPI structure, plan clarity, and exam accuracy. Study one specialty pattern per week: asthma, otitis media, fever, rash, abdominal pain, ADHD follow-up, well-child visit, sports injury, newborn feeding, or adolescent behavioral health. This steady loop turns training into expertise, especially when combined with future medical documentation trends, AI and automation in medical administration, voice recognition and dictation software knowledge, and AI medical scribe tool awareness.
6. FAQs About Becoming an Expert Pediatric Medical Scribe
-
Pediatric scribing is harder because the note depends on age-specific context, caregiver history, child behavior, vaccine status, growth and development, medication dosing, privacy issues, and detailed family instructions. A general complaint like cough, fever, vomiting, rash, or abdominal pain needs pediatric detail before it becomes clinically useful. You can build that foundation through top terms medical scribes must master, medical terminology for scribes, pediatric hiring network research, and scribe documentation accuracy reports.
-
You can apply without direct pediatric experience if you can show strong scribe fundamentals, clean medical terminology, EMR readiness, privacy awareness, and a serious understanding of pediatric visit patterns. A beginner with structured preparation often performs better than someone with vague healthcare exposure. Build readiness through medical scribe certification exam preparation, top scribe training courses and certifications, interactive scribe practice exams, and medical scribe career roadmap content.
-
Start with fever, URI, otitis media, asthma or wheezing, vomiting and diarrhea, dehydration, rash, abdominal pain, sore throat, allergies, lacerations, fractures, sports injuries, ADHD follow-ups, well-child visits, and newborn feeding concerns. These conditions teach the core pediatric pattern: age, onset, associated symptoms, intake, output, exposures, medications, exam, education, and return precautions. Pair condition study with ER scribing practice, urgent care scribe opportunities, primary care scribe networks, and specialty template libraries.
-
Use a repeatable pediatric HPI checklist: age, source of history, chief complaint, onset, duration, severity, progression, associated symptoms, pertinent negatives, exposure history, home treatment, last dose, intake, output, behavior, past history, allergies, vaccines, and caregiver concern. After each shift, review where your notes needed provider correction. That feedback loop is faster than passive studying. Strengthen it with scribe exam mistake prevention, real-life scribe exam questions, EMR charting terminology, and documentation accuracy analysis.
-
Pediatric scribes should understand HIPAA basics, guardian involvement, custody-sensitive communication, adolescent confidentiality, behavioral health documentation, portal access concerns, and clinic policy around sensitive topics. The safest professional habit is to follow provider direction, document clinical facts cleanly, and avoid casual assumptions about who can receive information. Study HIPAA terms for medical scribes, patient privacy communication essentials, HIPAA terms for administrative assistants, and healthcare portal terms.
-
A strong pediatric plan records what the provider told the family to do, what warning signs require urgent care, when to follow up, and how medication or supportive care should be handled. The best notes make the family’s next steps clear: fluids, fever control, inhaler use, wound care, school return, specialist referral, test follow-up, or escalation for worsening symptoms. Improve this skill through effective patient communication, active listening techniques, patient intake procedures, and de-escalation techniques.
-
AI tools are changing documentation, but pediatric notes still need human judgment support around context, family dynamics, age-specific details, privacy-sensitive history, and provider-specific plan language. A scribe who understands AI tools, ambient dictation limits, EMR workflows, and clinical documentation quality becomes more valuable in hybrid documentation environments. Study AI medical scribe tools, future medical documentation trends, voice recognition software, and AI automation in medical administration.